Problems with chewing, teeth rustling and articulation? Cracking, pain, tooth loosening? Headaches ? Functional imbalances? As common as they may be, problems with dental occlusion, which defines how the upper and lower teeth fit together, should not be taken lightly. Malocclusion can not only lead to chewing problems, but also have serious physiological and psychological consequences: it affects the smile, as well as visual acuity, sleep or body posture, from head to toe.
There are several types of malocclusion, also called occlusal dysfunction, which vary according to the direction of the alignment of the teeth. The most common type of dental malocclusion is the inverted dental occlusion, or inverted articulated malocclusion. Their orthodontic treatment can be difficult and expensive. In The UK, the NHS reimburses 100% of treatments for children under 18 years old, but adults are not so lucky: their operation can only be covered for grade 4 and 5 cases, grade 3 are judged on individual basis.
For some adults who, for various reasons, have not been able to treat their dental malocclusion in time, dental tourism is an obvious alternative. Turkey has become a world-class destination for dental work. Its dental clinics, especially in Istanbul, the country’s cultural, tourist and economic capital, have an international reputation for the excellence of their care and their dental surgeons, offering patients from all over the world a very attractive quality/price ratio.
What is dental occlusion?
Dental occlusion is the way the teeth of the two jaws fit together, the lower mandibular teeth and the upper maxillary teeth. A good dental occlusion allows perfect chewing and swallowing, while ensuring good phonation (production of sounds for speech) and good postural balance. Numerous scientific studies on the subject have shown the fundamental importance of the physiological resting posture of the mandible in relation to the jawbone, during which the muscular contraction of the entire body is weak and symmetrical, stable and repetitive. In yoga, for example, a good meditation posture involves the tongue touching the top of the palate to ensure proper rest of the manducatory muscles and complete body inertia.
A perfect dental bite is rare, as most humans do not have perfect alignment of their teeth. An acceptable, or normal, bite reveals some imperfections (slight overlap, rotation of some teeth), but allows the teeth to function properly. Properly aligned teeth allow for a brighter smile, are easier to clean, and slow down the formation of cavities or gingivitis. When problems are more serious, we talk about dental malocclusion.
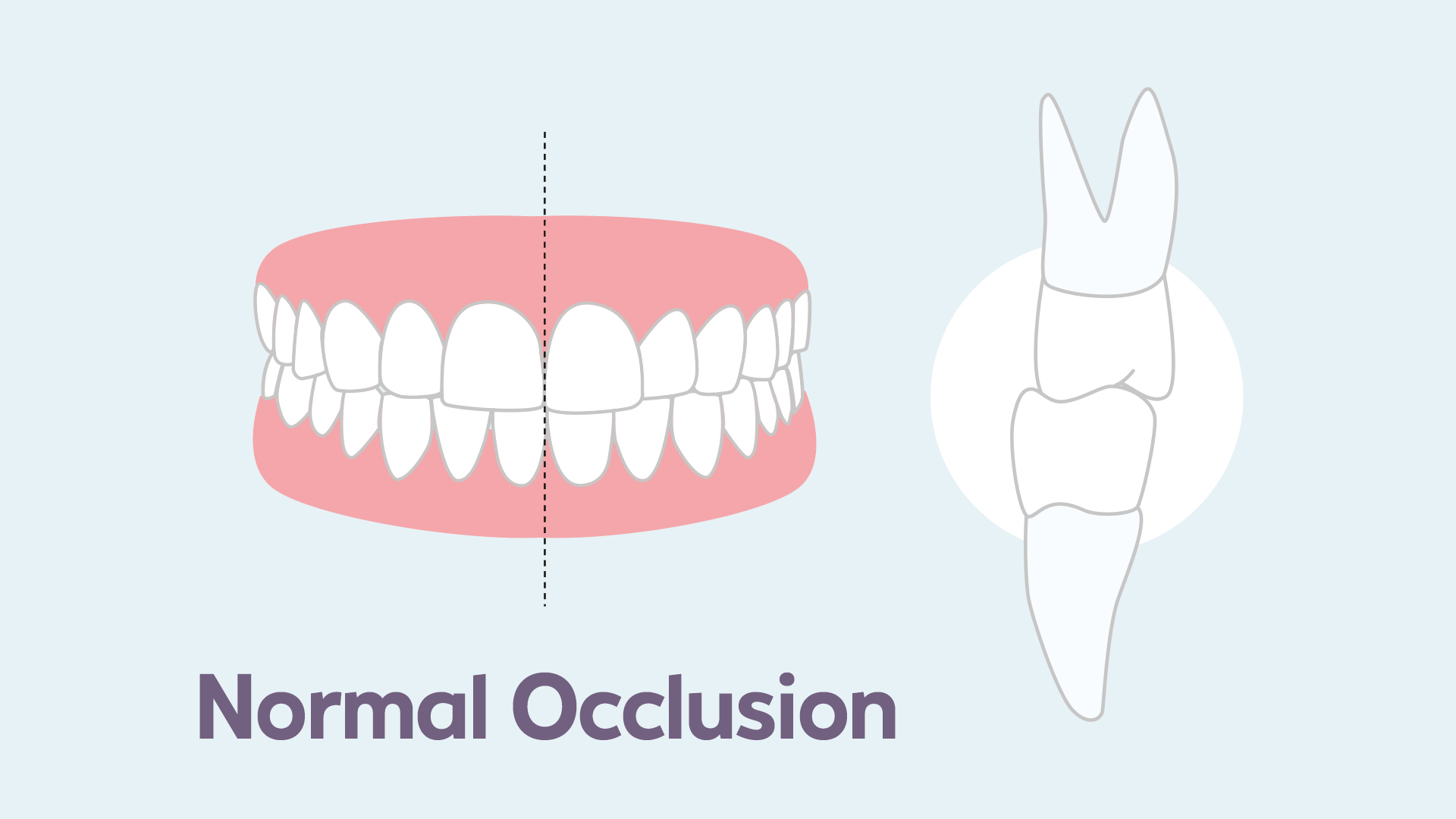
What characterizes malocclusion?
As the name implies, a dental malocclusion is characterized by an imperfect dentition that prevents or disturbs the proper assembly of the upper teeth with the lower ones, hindering the muscular function of the jaws. Symptoms of dental malocclusion include incorrect alignment, changing facial expressions, frequent biting of the inside of the cheeks or tongue, impaired chewing, slurred speech, breathing through the mouth rather than the nose, and even chronic headaches. Experts refer to TMJ disorders when an occlusal dysfunction disrupts the proper functioning of the temporomandibular joints (TMJ), the two joints between the lower jaw (mandible) and the skull. These TMJ disorders can be the cause of many physiological and psychological problems (fatigue, migraines, speech problems, etc.).
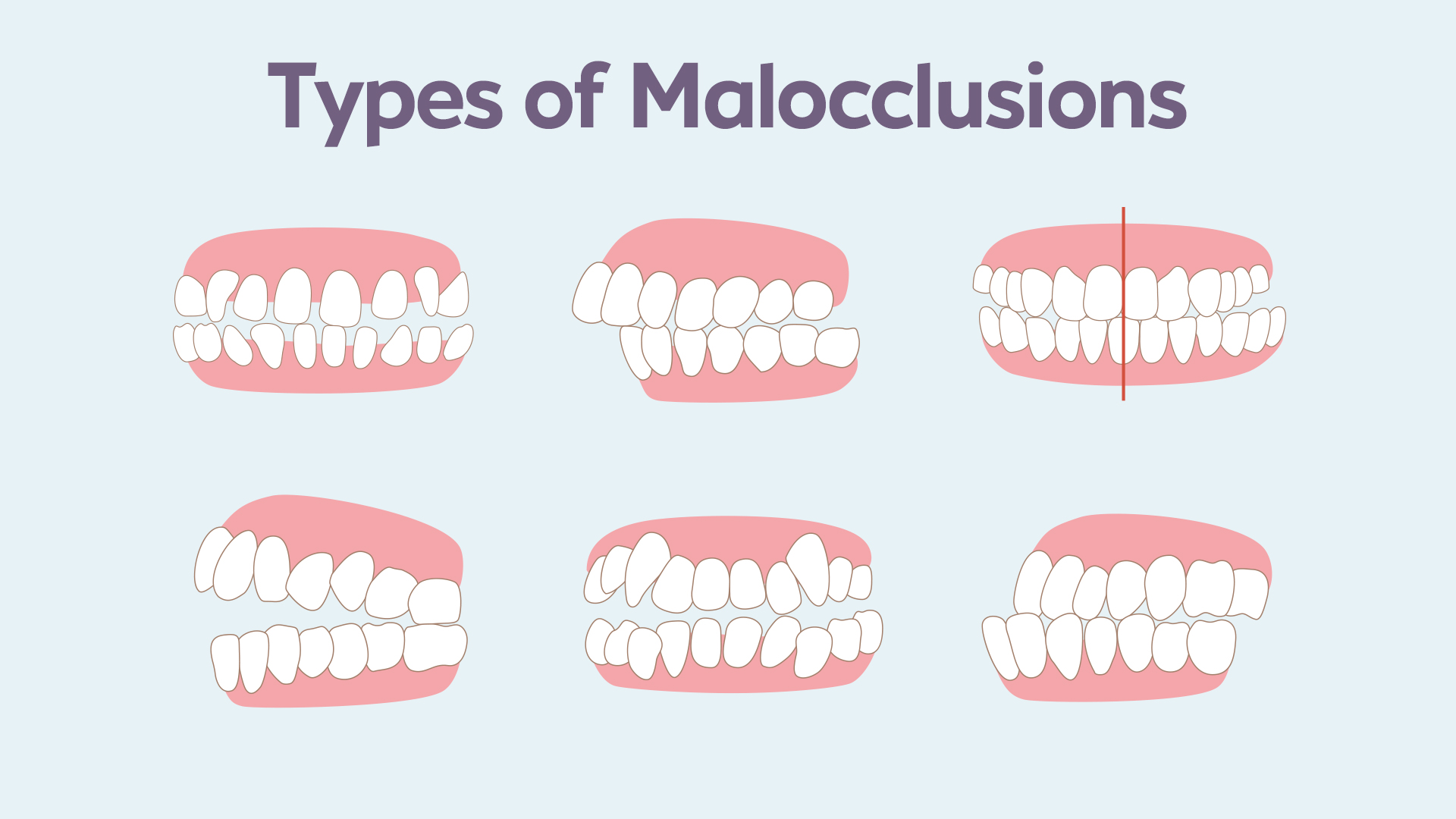
The different types of malocclusion
There are many different forms of dental malocclusion, which specialists divide into classes 1, 2 and 3. Each class is characterized by the type of relationship between the upper and lower molars.
- Class 1 malocclusion: the most frequent malocclusion, affecting between 50 and 60% of young people between the ages of 6 and 17. In this case, the molars fit together correctly, but the other teeth do not align well: overlapping of the anterior teeth and crowding of the upper or lower incisors and canines, protruding maxillary incisors with spaces between the teeth, anterior or posterior crossbite, or lack of space for normal growth of the posterior teeth, canines, and/or premolars
- Class 2 malocclusion: when the upper molars are malpositioned in relation to their lower twins, either forwards or backwards, this leads not only to problems with chewing, but also with the design of the face and mouth. The lips can be misplaced, with the lower lip coming under the upper incisors and canines, with a chin behind, or on the contrary, coming up in front of the upper lip. Corrections of class 2 malocclusions often allow for correction of the smile.
- Class 3 malocclusion (severe malocclusion): the rarest cases are classified in this category. In particular when the lower molars are too far forward in relation to the upper molars. This is called prognathia (advanced lower jaw), sometimes characterized by a chin that is too far forward, or a receding upper jaw. When all the lower teeth overlap the upper ones, this malocclusion is called inverted occlusion, or global inverted bite. A dental imbalance that will strongly hinder chewing, prematurely wear out the teeth and spoil the smile, but can also lead to postural problems (neck pain, back pain, tinnitus…).
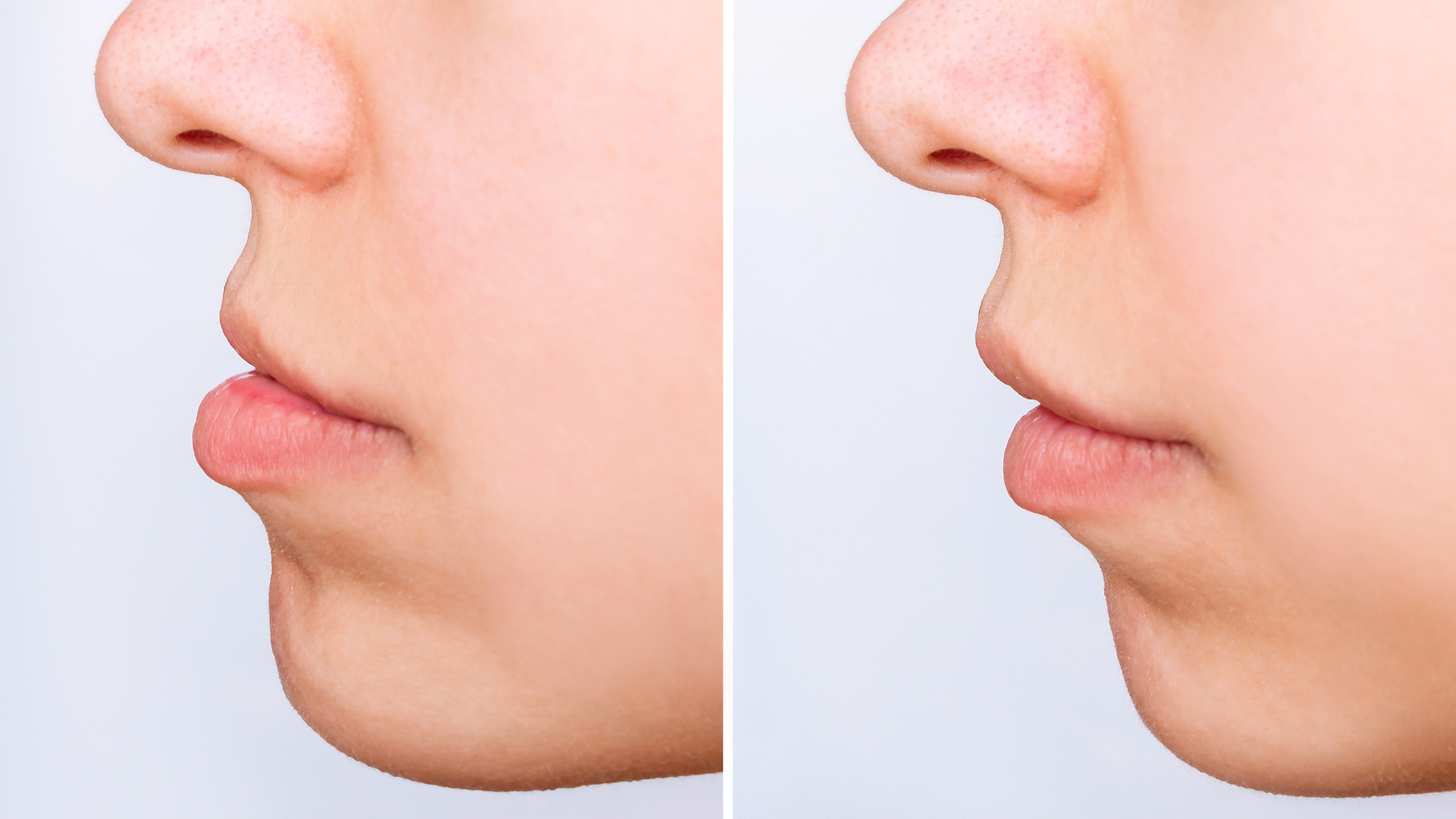
Possible causes of a malocclusion
The causes of dental malocclusion are varied. It can often be linked to the patient’s genetic heritage, but not only. It can appear after a recurrent infantile behavior (salivary deglutition, sucking of thumb or pacifier, etc…) or an accident (fall of tooth…).
- Atypical salivary deglutition during childhood, which would affect more than 75% of children, leading to an insidious migration of teeth (backwards or forwards).
- Incorrect jaw posture reducing the physiological resting time
- Uncontrolled or uncompensated dental extractions with the growth of healthy teeth or wisdom teeth
- Damaged teeth causing an inocclusion or an underbite (antagonistic teeth no longer touching)
- Late orthodontic treatment
- Maxillary surgery coupled with poor rehabilitation of the manducatory muscles.
The aggravating factors of malocclusion
A damaged dental occlusion can lead to a malocclusion several years later. This is why it must be diagnosed, characterized and treated as soon as possible in children and adolescents, especially during the growth period, to prevent it from worsening. Here are the main aggravating factors of a malocclusion:
- Chewing gum
- Sleeping on one side only
- Eating too hard
- biting your nails
- Not protecting your jaws during violent sports
- Do not apply ice to the TMJ area in case of trauma to the jaw.
The physical and psychological consequences of malocclusion
The effects of a dental malocclusion are numerous, and not only for the teeth: the postural muscles and the “reflex” nervous circuits that control these muscles can suffer the consequences. Some of these concerns lead to permanent exhaustion, which can disrupt a patient’s social relationships, without medical consultations providing an answer or remedy. Isolation and depression can set in, leading the patient into a tragic spiral. Occlusal dysfunction is believed to be one of the primary causes of Costen’s syndrome, which is the source of many undiagnosed health problems such as chronic migraines, vertigo, neck pain and hearing problems. Here is a non-exhaustive list of these symptoms.
- Imbalance in the opening/closing of the mandible
- Aseptic dental necrosis
- Dental loosening
- Breathing difficulties
- TMJ disorders (temporomandibular joints)
- Postural disorders in the cervical muscles and shoulders
- Myalgias (muscle pain and cramps)
- Chronic fatigue, depression
- Postural imbalance leading to musculo-tendinous problems (contractures, strains, sprains, tendinitis, arthritis, arthrosis…)
- Headaches, headaches, migraines
- Snoring, sleep apnea, tinnitus
- Tachycardia…
Possible treatments for malocclusion
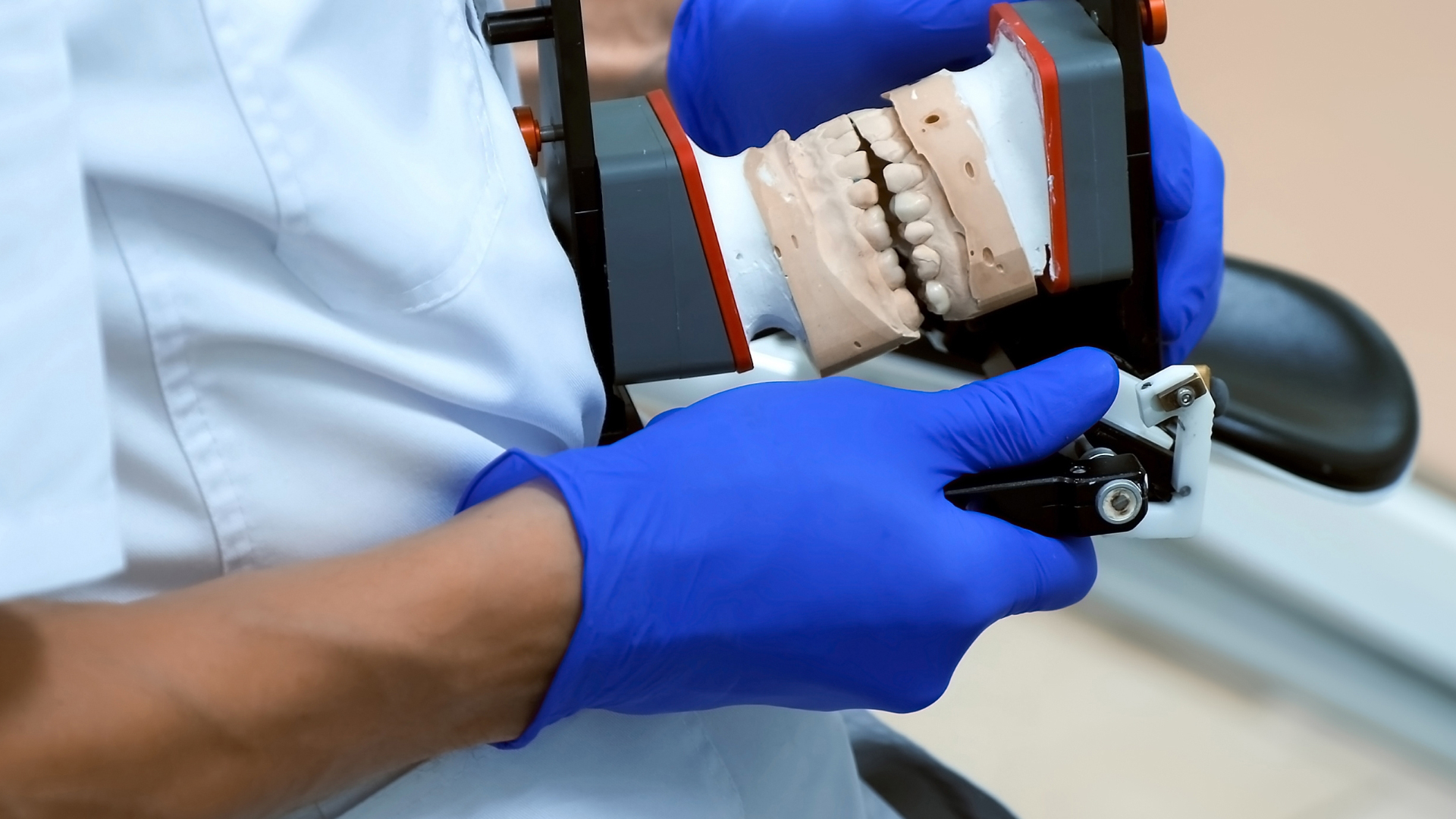
Dental bite problems can be diagnosed by a dentist, orthodontist or osteopath practicing dentofacial orthopedics. An X-ray will give an overview of the alignment of the teeth and the configuration of the jaw, while an MRI (Magnetic Resonance Image) will help to detect any abnormalities around the meniscus (which ensures the mobility of the jaw during chewing) and the ligaments of the joint. The patient’s examination is not limited to the jaw: his or her postural balance and the study of the neck muscles will help to perform an occlusal analysis and clarify the diagnosis.
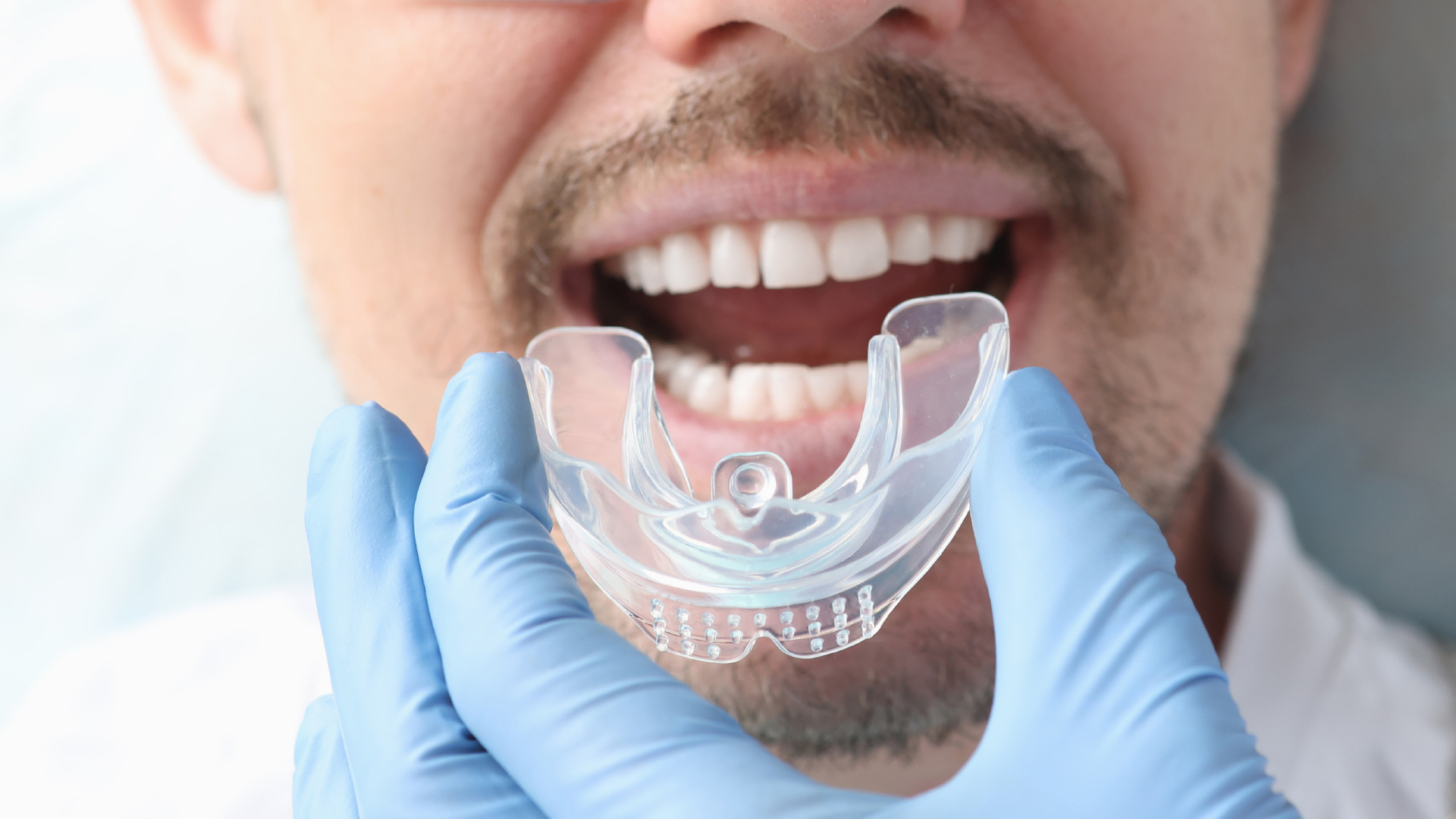
Once the malocclusion has been diagnosed, treatment may consist of braces or removable aligners such as Invisalign®. Selective grinding of the teeth, to restore their ideal spacing, is also possible, accompanied by crowns and/or veneers to make this grinding invisible. At the same time, the patient can undergo osteopathic treatment, or even relaxation methods, to eliminate muscular problems, back pain or migraines. Finally, for more serious procedures, especially for class 2 or 3 malocclusion, maxillofacial surgery will play a fundamental role, allowing the jaws and their teeth to be replaced in an ideal way. These operations can be performed under local anesthesia when it is limited to extractions and dental implants, but also, under general anesthesia when surgery of the jaws is required. The patient will regain a normal occlusion and a radiant smile.

Malocclusion treatment: before and after


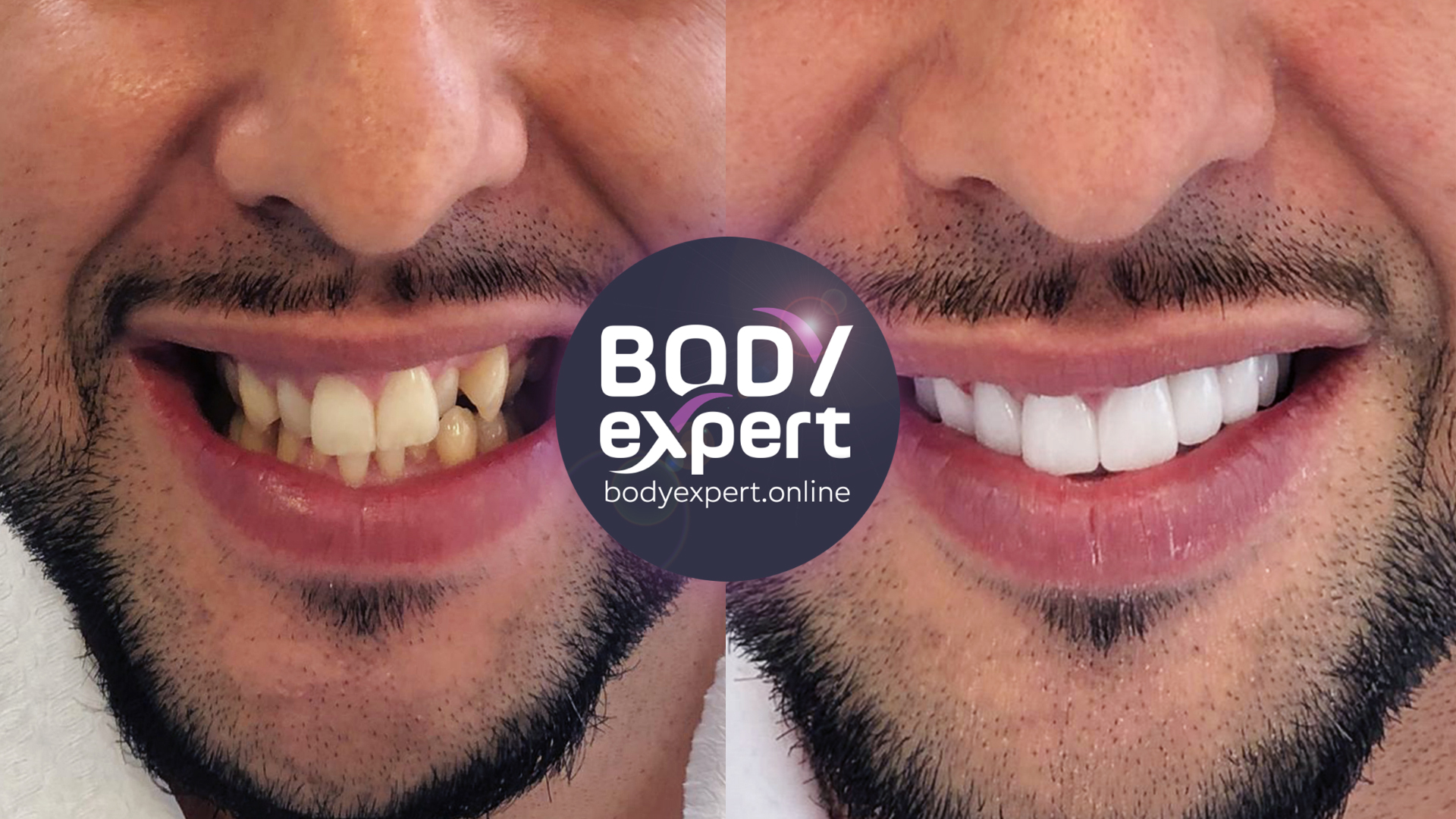
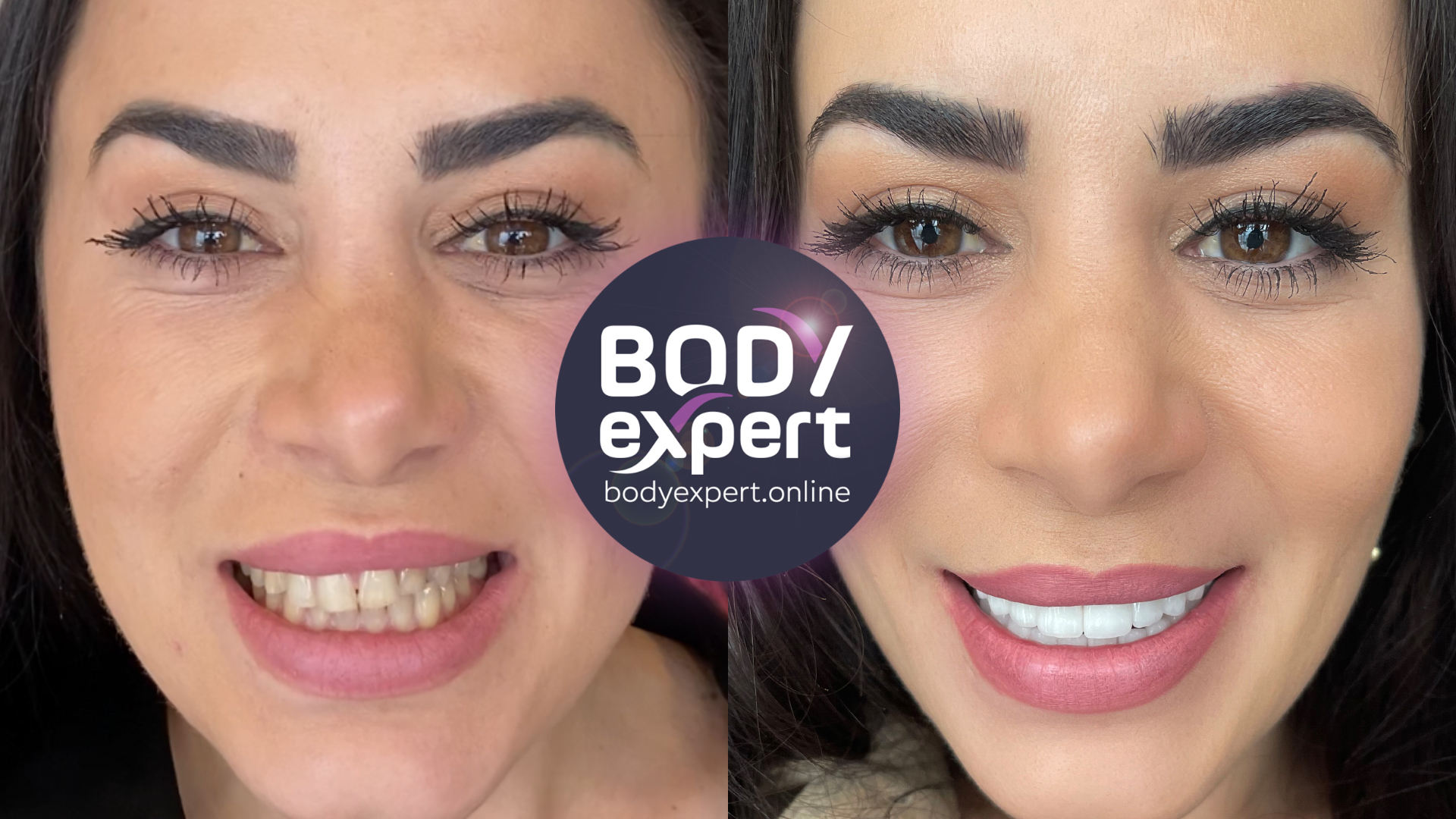

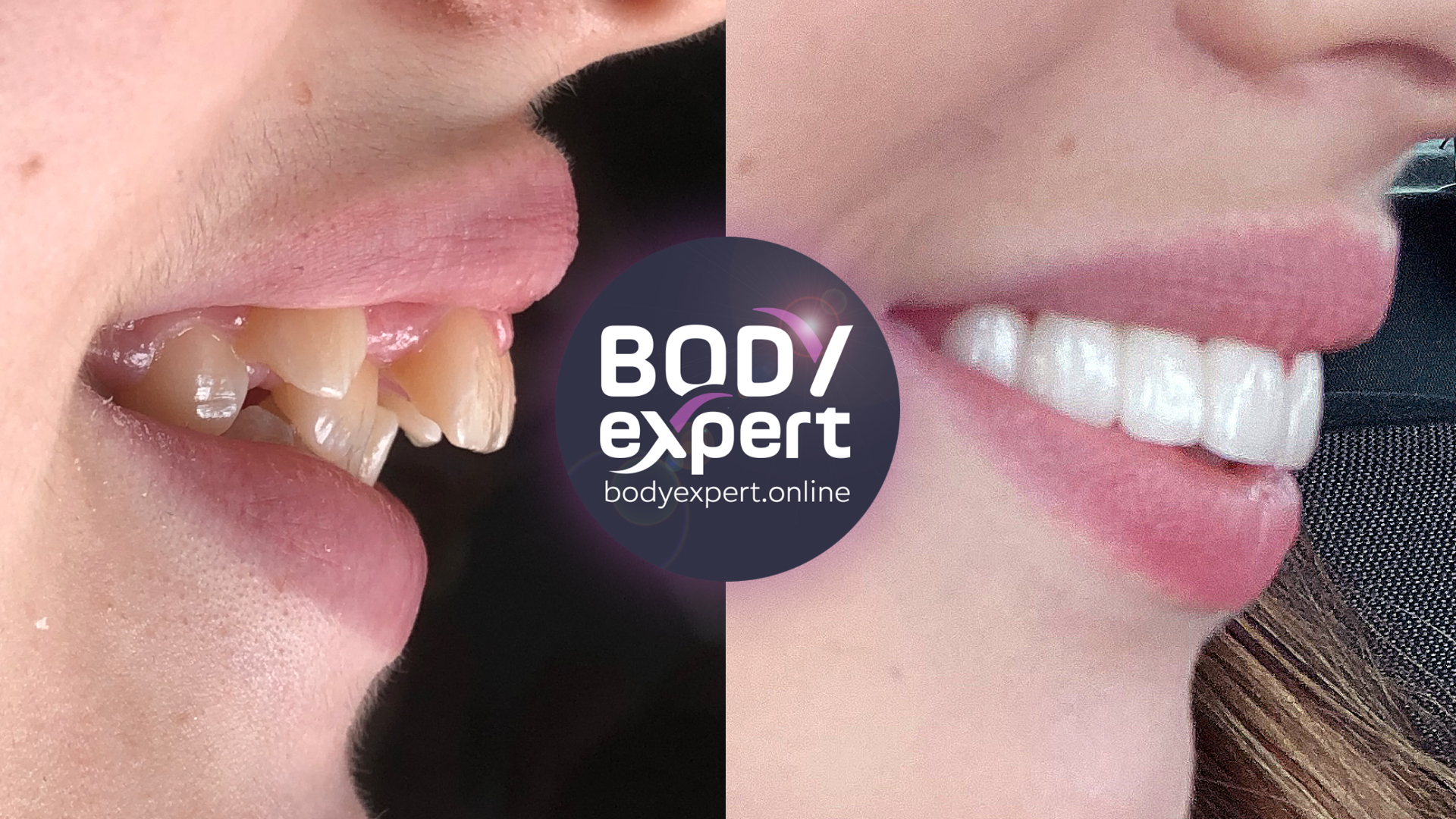
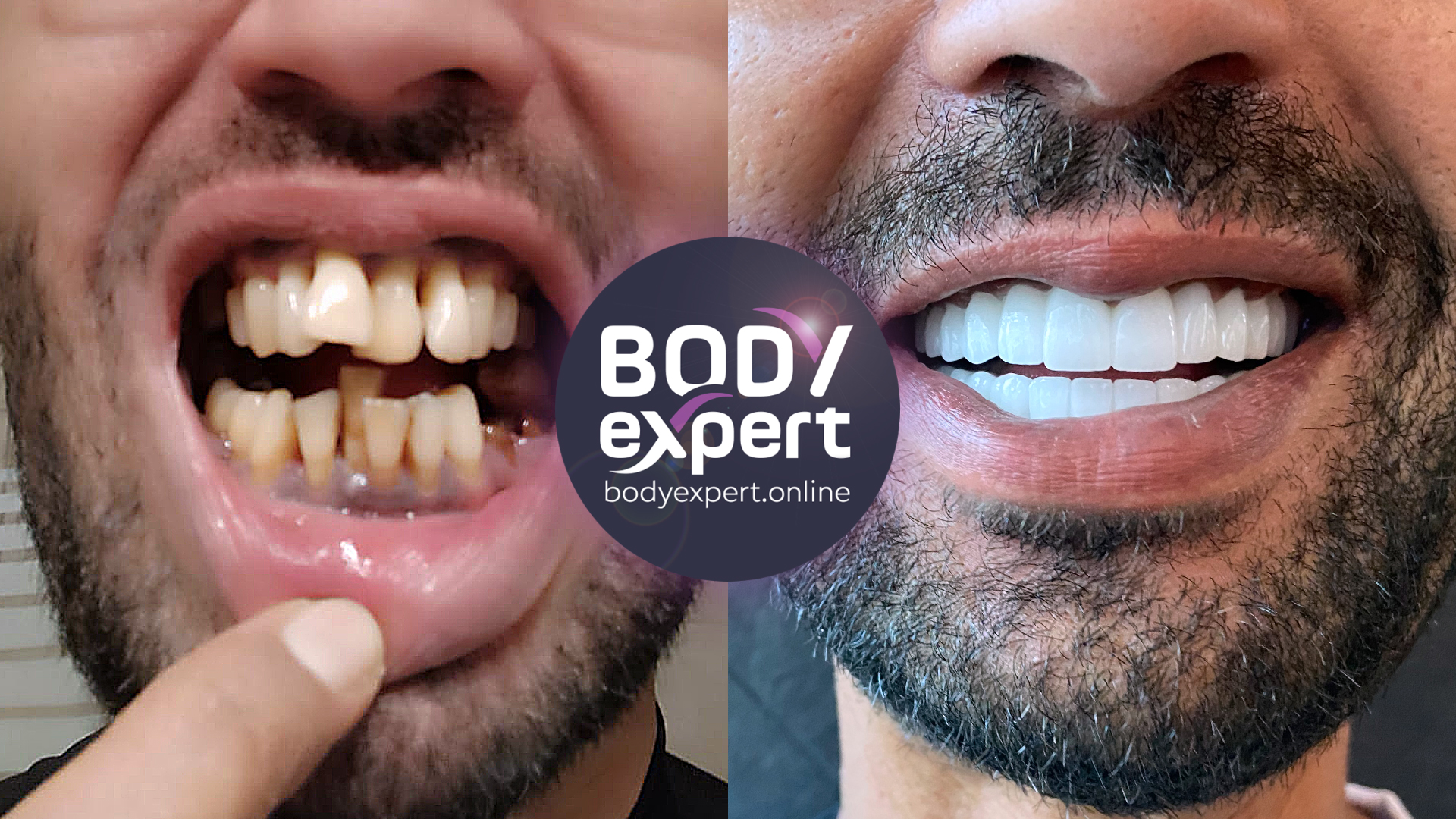
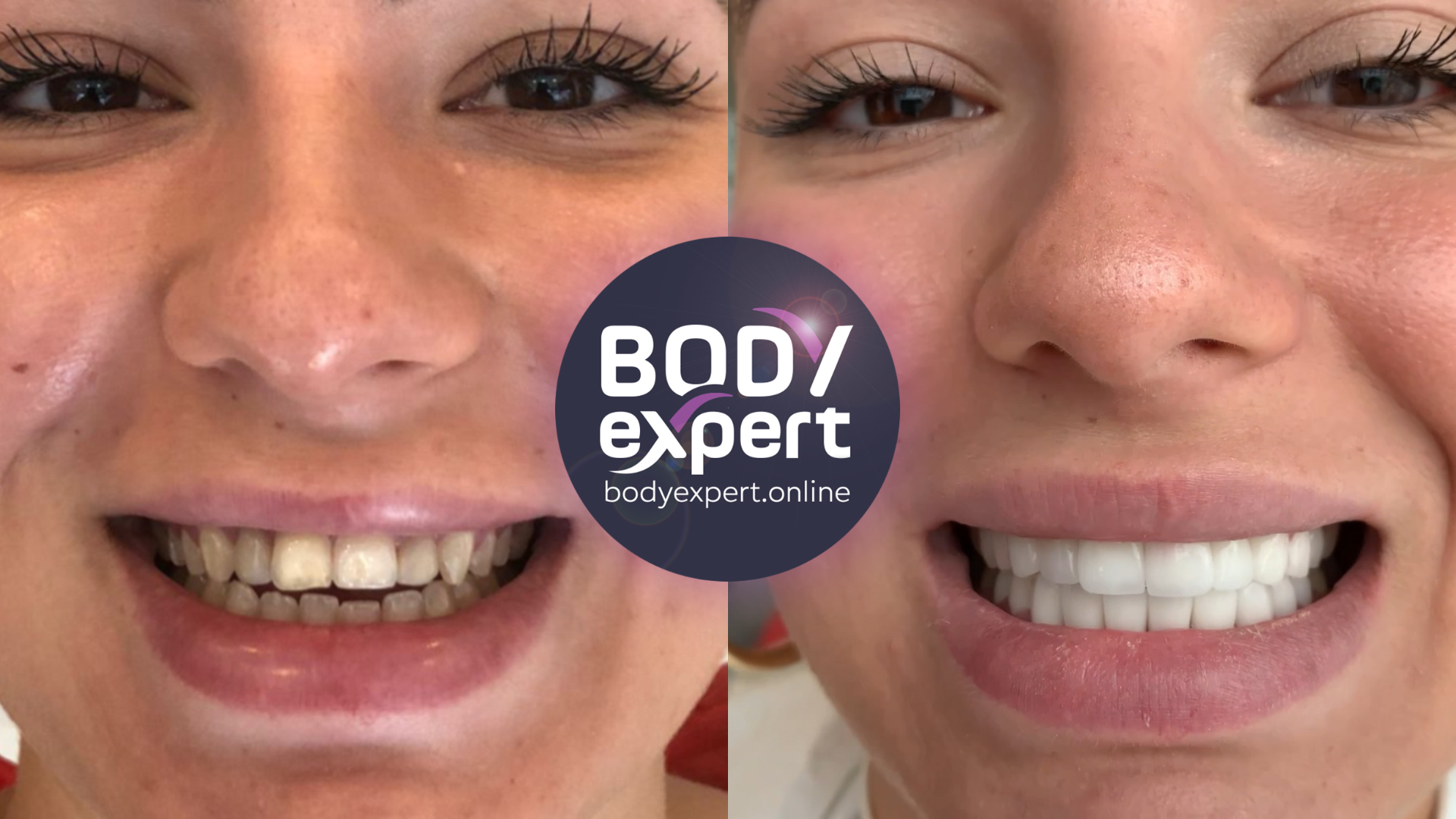
Dental malocclusion: testimonials
40266 vues
0 commentaires
0



Il n'y a pas de commentaires pour le moment.